 Although fairly wide-spread, much is still unknown about vitiligo including its causes and treatment. In this article, we’ll have a look at vitiligo-research published in the last few months.
Although fairly wide-spread, much is still unknown about vitiligo including its causes and treatment. In this article, we’ll have a look at vitiligo-research published in the last few months.
With regards to cause, on July 18, 2019, the American Journal of Human Genetics published a study that revealed that both genetic and environmental factors play significant roles in the onset of vitiligo. This gave scientific confirmation on what I’ve long suspected – that genetics are only part of the story. Scientists found that the vitiligo genetic score is higher in multiplex families than in simplex cases (no family history of vitiligo). The more family members have vitiligo, the higher the risk of developing this skin condition[i]. Diet is crucial in vitiligo (read more: Saturated Fat & Vitiligo)
Bearing in mind the exact mechanisms associated with the onset and formation of vitiligo is complex, many studies are focused on this subject. A study published on January 2, 2020, in the Australasian Journal of Dermatology confirmed that people with vitiligo had increased presence of pro-inflammatory cytokine[ii], interleukin (IL)-17. This shows that inflammation could also play a role in the onset and development of this common skin condition. The discovery could also help develop new treatments for vitiligo and confirms what I long believed that inflammation plays an important role in this disease. This is the reason why turmeric is an effective treatment option, because it has potent anti-inflammatory action. Read more: Turmeric – a novel approach to curing vitiligo.
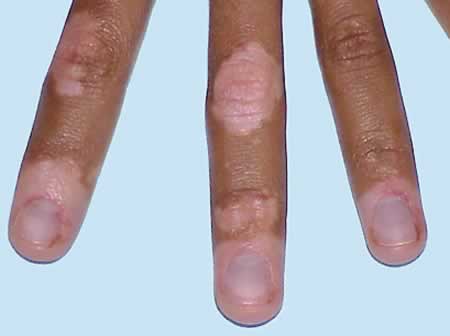
Patients with vitiligo have a higher level of circulating autoantibodies specific to melanocyte cytoplasm and surface antigens associated with the extent of the condition. A study published in January-February 2020 issue of the Indian Journal of Dermatology aimed to evaluate the role of antimelanocyte antibodies, complement 3 and 4 (C3 and C4, and antinuclear antibodies in vitiligo pathogenesis. The results showed that levels of antinuclear antibodies, antimelanocyte antibodies, and C4 are higher in vitiligo patients. The scientists concluded that antimelanocytes have a role in the pathogenesis of vitiligo[iii], but more studies on this subject are necessary to uncover as much as possible on their influence on the common skin condition.
Research from the Journal of the American Chemical Society shed some light on the common therapy used to treat skin diseases, including vitiligo. PUVA, short for psoralen UVA, is primarily used to treat vitiligo and psoriasis. The study, published on August 15, 2019, showed that after the psoralen molecule has absorbed UV light, the reaction takes place in two stages. The first stage involves the formation of a single bond between psoralen and thymine, and it occurs within a microsecond while the second phase takes place in 50 microseconds. Understanding of PUVA therapy could allow scientists to change psoralens chemically in a targeted way to make the treatment more effective[iv].
There was also a study looking at herbal therapy. In this research from Dermatologic Therapy, it was reported that black cumin or Nigella sativa could indeed help with re-pigmentation. The study, published on May 6, 2019, included 33 vitiligo patients who applied a cream containing N. Sativa seed oil on the hands, face, and genital region two times a day for six months. Statistically, significant repigmentation was observed in treated areas. This led scientists to concluded that Nigella sativa could be used as an adjuvant therapy that contributes to the treatment of vitiligo, particularly in sensitive areas such as the genital region[v].
Speaking of treatment of vitiligo, on January 20, 2020, the Expert Opinion on Emerging Drugs published a study that explained that treatment of this condition needs to be multimodal. Topical and oral JAK inhibitors are the most promising new class of drugs currently available for the treatment of vitiligo and work best in combination with NB-UVB[vi]. JAK inhibitors, short for Janus Kinase inhibitors, are widely explored for their benefits to treat inflammatory conditions.
Written by Michael Dawson – nutritionist, health consultant, and author of Natural Vitiligo Treatment System: The Home Vitiligo Cure that Doctors Don’t Want You to Discover.
Check out the Vitiligo 2022 UPDATE here <==
References:
[i] Spritz RA, Roberts GHL, Paul S, et al. Family clustering of autoimmune vitiligo results principally from the polygenic inheritance of common risk alleles. The American Journal of Human Genetics 2019 Jul;105(2):364-372. DOI: https://doi.org/10.1016/j.ajhg.2019.06.013
[ii] Acharya P, Mathur M. Interleukin-17 level in patients with vitiligo: A systematic review and meta-analysis. Australian Journal of Dermatology 2020 Jan. DOI: https://doi.org/10.1111/ajd.13233
[iii] El-Gayyar MA, Helmy ME, Gaballah MA, et al. Antimelanocyte antibodies: A possible role in patients with vitiligo. Indian Journal of Dermatology 2020 Jan-Feb; 65(1):33-37, DOI: https://doi.org/10.4103/ijd.IJD_344_18
[iv] Diekmann J, Gontcharov J, Frobel S, et al. The photo addition of psoralen to DNA proceeds via the triplet state. Journal of the American Chemical Society 2019 Aug;141(34):13643-13653, DOI: https://doi.org/10.1021/jacs.9b06521
[v] Sarac G, Kapicioglu Y, Sener S, et al. Effectiveness of topical Nigella sativa for vitiligo treatment. Dermatologic Therapy 2019 Jul;32(4):12949, DOI: https://doi.org/10.1111/dth.1249
[vi] Karagaiah P, Valle Y, Sigova J, et al. Emerging drugs for the treatment of vitiligo. Expert Opinion on Emerging Drugs 2020 February 3:1-18, DOI: https://doi.org/10.1080/14728214.2020.1712358