Vitiligo is a chronic skin pigmentation that causes the development of white or lighter patches of skin. These patches can appear anywhere on the body. Other signs and symptoms can also be associated with this condition. While vitiligo on its own is not a life-threatening disorder, its early diagnosis and timely management are essential for preventing its complications and related health risks.
A vitiligo diagnosis typically consists of the history of your signs, symptoms, past medical history, general physical examination, a specific examination of the skin, and, potentially, a skin biopsy or blood tests. It is also important to rule out other conditions. Doctors will also evaluate for other health conditions as vitiligo increases the risk of having other auto-immune disorders along with it.
Self-Checks
Though there are no at-home tests recommended for the diagnosis of vitiligo, you can examine your skin carefully and look for white or clear patches on your skin, hair, and eyes. These white or lighter patches are the main symptoms of vitiligo, and they are clearly visible on the skin. Keeping a close eye on your skin regularly can help you spot the symptoms early and seek early management.
Here are some of the most common symptoms that you can check your skin for:
- Patchy or widespread loss of skin color
- Early whitening of the hair on your head, eyelashes, and eyebrows
- Loss of color on the inside of your mouth or nose
- Pain, itching, or discomfort on the affected areas of skin
Medical History
Diagnosis of the vitiligo in the doctor’s office would start with the complete history of your signs and symptoms. Your dermatologist will likely cover the following points:
- Complete details of your signs and symptoms, including their time of onset, their location, and their pattern of spreading
- Family history of vitiligo
- Family history of other autoimmune disorders such as rheumatoid arthritis (RA), lupus, or thyroid disease
- Any skin problems previously
- General health, including physical, mental, and emotional wellbeing
Physical Examination

After taking a complete history of your symptoms, your dermatologist will start the general physical examination and the examination of your skin. This skin examination would be different and more elaborate than the self-checks you may have done at your home.
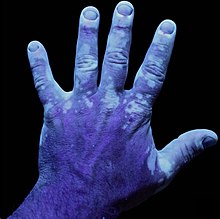
The doctor will note the location of the patches, their size, their pattern, and their symmetry. Mostly, the doctor will be using special light known as a Wood’s lamp to check if the white or light patches are vitiligo.
If doctors need more information before finalizing a diagnosis, they may run some blood tests or perform a skin biopsy to determine any underlying condition.
Skin Biopsy
A skin biopsy involves the removal and evaluation of a small portion of the affected skin tissue under a microscope in the lab. If a microscope shows that there are no pigment cells present, a diagnosis of vitiligo may be considered final. A skin biopsy will also help to rule out any skin cancer as some types of skin cancers, such as hypopigmented cutaneous T-cell lymphoma may cause white patches that look similar to vitiligo patches.
Blood Tests
Your doctor may run some blood tests to assess your overall general health and to address specific areas of concern, such as your thyroid function. Common blood tests ordered in Vitiligo are:
- Complete blood count (CBC)
- Antinuclear antibody (ANA) test
Eyesight or Hearing Examinations
As vitiligo can affect your eyes and hearing, your dermatologist may seek the opinion of or may refer you to an ophthalmologist or audiologist for further assessment of eye-related or hearing-related symptoms.

References
- Gawkrodger, D. J., Ormerod, A. D., Shaw, L., Mauri-Sole, I., Whitton, M. E., Watts, M. J., Anstey, A. V., Ingham, J., Young, K., Therapy Guidelines and Audit Subcommittee, British Association of Dermatologists, Clinical Standards Department, Royal College of Physicians of London, Cochrane Skin Group, & Vitiligo Society (2008). Guideline for the diagnosis and management of vitiligo. The British journal of dermatology, 159(5), 1051–1076. https://doi.org/10.1111/j.1365-2133.2008.08881.x
- Gawkrodger, D. J., Ormerod, A. D., Shaw, L., Mauri-Sole, I., Whitton, M. E., Watts, M. J., Anstey, A. V., Ingham, J., & Young, K. (2010). Vitiligo: concise evidence based guidelines on diagnosis and management. Postgraduate medical journal, 86(1018), 466–471. https://doi.org/10.1136/pgmj.2009.093278
- Ezzedine, K., & Silverberg, N. (2016). A Practical Approach to the Diagnosis and Treatment of Vitiligo in Children. Pediatrics, 138(1), e20154126. https://doi.org/10.1542/peds.2015-4126
- Kumar Jha, A., Sonthalia, S., Lallas, A., & Chaudhary, R. (2018). Dermoscopy in vitiligo: diagnosis and beyond. International journal of dermatology, 57(1), 50–54. https://doi.org/10.1111/ijd.13795
- Boissy, R. E., & Nordlund, J. J. (2011). Vitiligo: current medical and scientific understanding. Giornale italiano di dermatologia e venereologia : organo ufficiale, Societa italiana di dermatologia e sifilografia, 146(1), 69–75.