Vitiligo is a common skin disorder that causes painless, white patches to appear on the skin. The exact cause is unknown; however, it is considered an auto-immune condition with genetics and family history playing a role as well (1). It occurs when the pigment-producing cells of the skin—known as melanocytes—stop functioning. As a result, white patches appear, which keep increasing in size with time. Vitiligo affects about 0.5 to 2% of the population worldwide (1).
Medical Conditions That Are Not Vitiligo!
Many skin conditions may be mistaken with vitiligo. Some of these have true white spots, but mostly they are hypopigmented and not depigmented like vitiligo.
These medical conditions may include:
Pityriasis Alba: A common condition in children, pityriasis alba first develops as red, scaly patches on the cheeks, front of elbows, and back of knees. When these patches heal, they turn into hypo-pigmented, light-colored spots. The exact cause of pityriasis alba remains unknown, and there is no treatment. The doctor may recommend a moisturizer cream as it often co-exists with dry skin.

Tinea Versicolor: It is a fungal infection that causes lighter spots on the chest and back. It is not dangerous and develops due to poor hygiene in a warm environment. It commonly affects children and is easily treated with an antifungal cream.
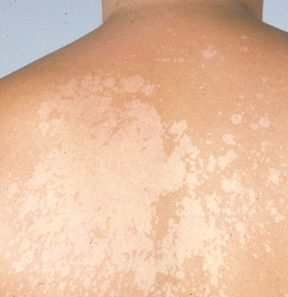
Chemical Leukoderma: It occurs due to the repeated exposure of skin to certain chemicals, such as phenol. Chemical exposure leads to loss of melanocytes, resulting in irregularly shaped discolored spots. It is not threatening and resolves with time. The doctor may recommend a topical corticosteroid with advice to avoid the allergen.
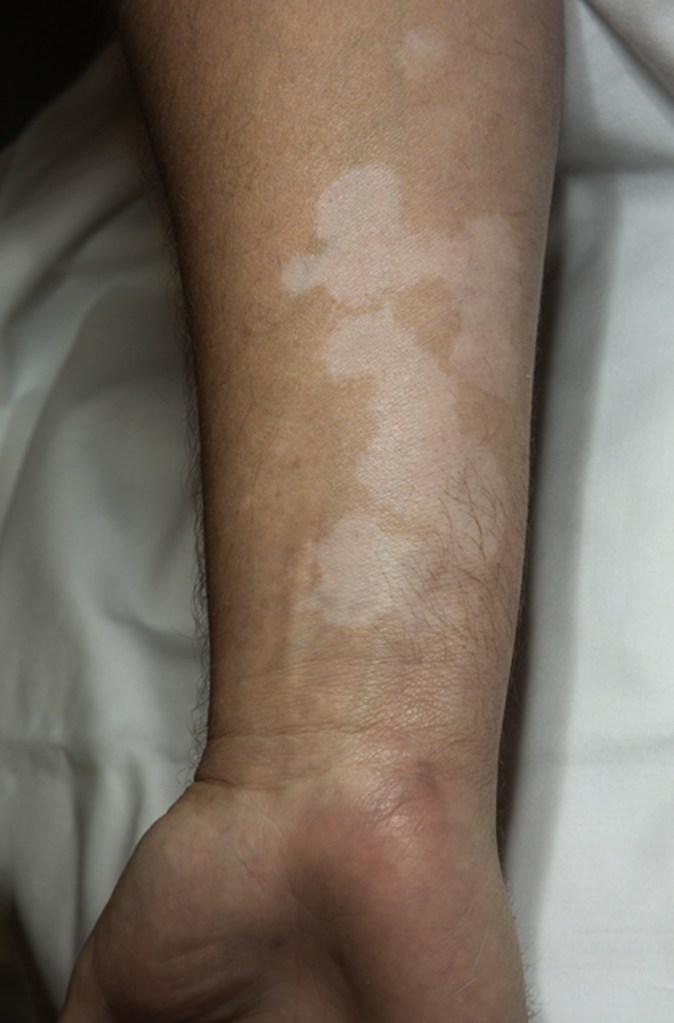
Piebaldism: It refers to the lack of melanocytes in an area of the skin, resulting in white skin and hair patches. It is a rare, inherited disorder present at birth and affects the front of the body. Most people have cosmetic concerns and follow cosmetic procedures to get rid of piebaldism.
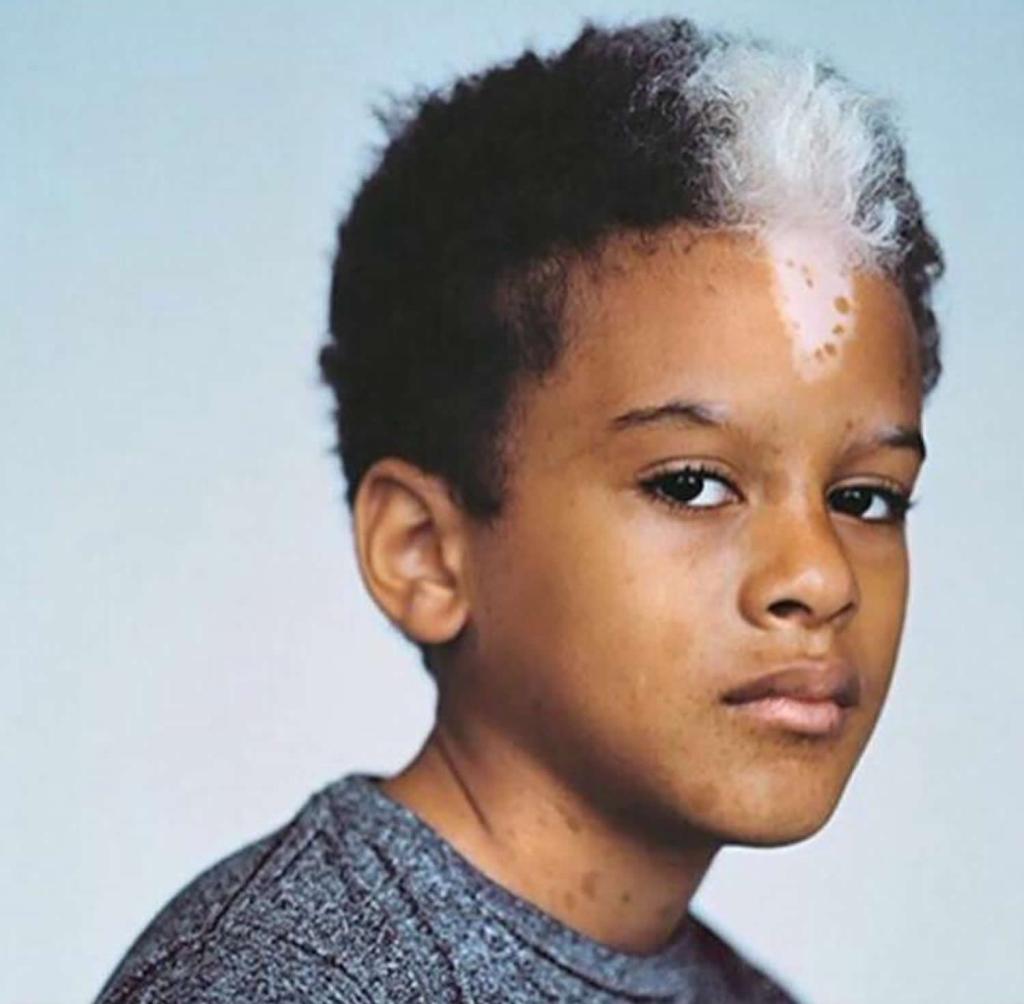
Nevus Depigmentosus: It is a birthmark that appears in the first few months of life. It is usually single but may present as multiple streaks. The hypopigmented skin patch does not grow in size, and unlike piebaldism, it does not turn the hair white either. People usually follow cosmetic procedures to eliminate nevus depigmentosus.
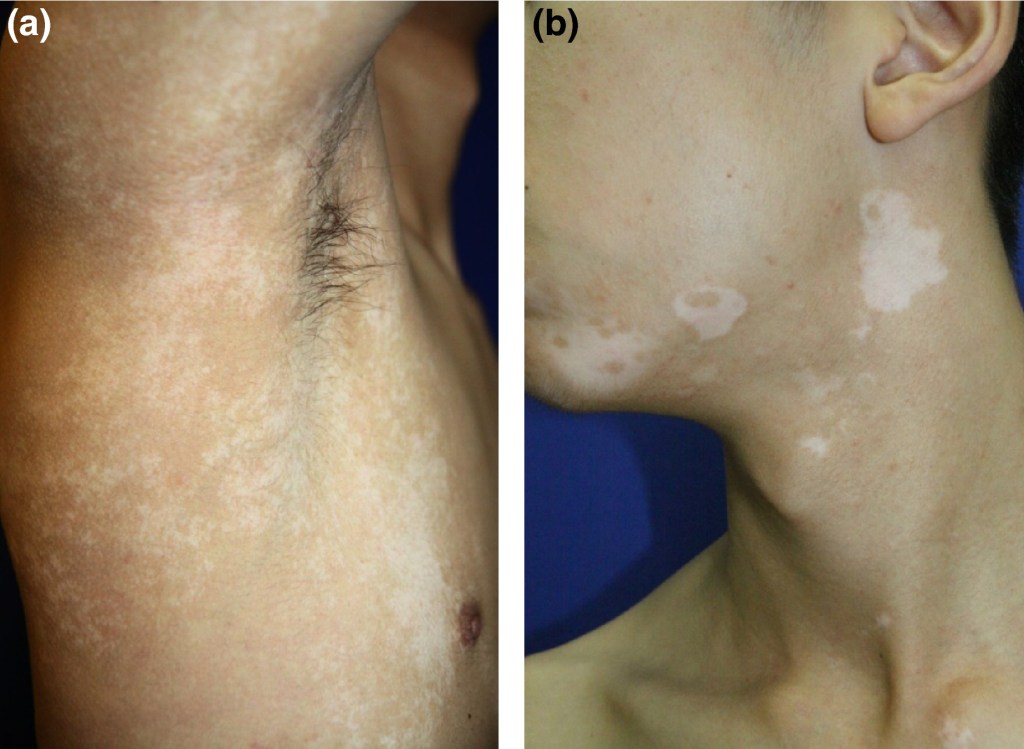
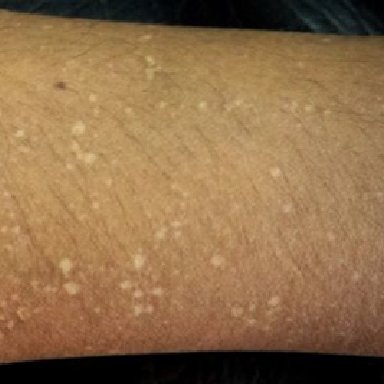
Idiopathic Guttate Hypomelanosis: It is characterized by many oval or round hypopigmented spots on the exposed surfaces. It occurs due to chronic sun exposure and usually involves the shins, forearms, and sometimes, chest and back. No treatment is necessary; however, the doctor may prescribe topical steroids following the patient’s concerns.
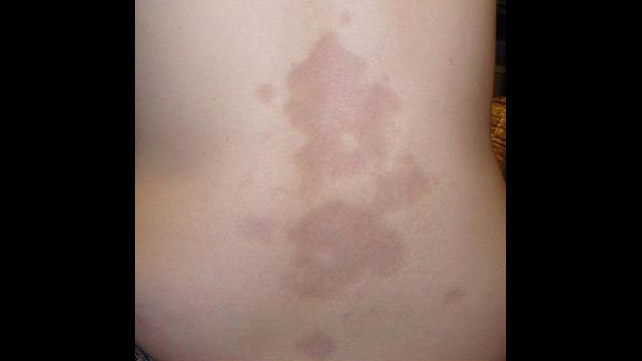
Morphea: Morphea is the excessive collagen deposition on one or more areas of the skin, leading to painless, discolored patches. It is considered auto-immune and involves thickening and hardening of the skin. Treatment is necessary to avoid permanent skin changes and involves phototherapy and immune-suppressive medications.
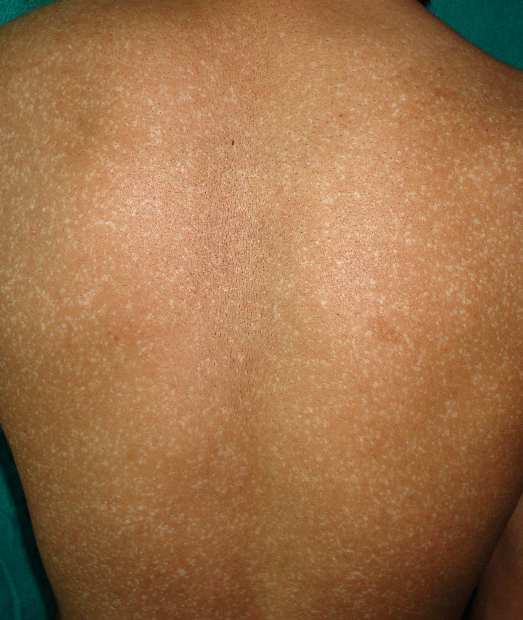
Progressive Macular Hypomelanosis: It commonly affects the females and looks like tinea versicolor, however, without scales. It presents as pale circular skin patches at the front and back of the trunk and does not require treatment. The doctor may recommend phototherapy and a combination of other therapies following patients’ concerns.
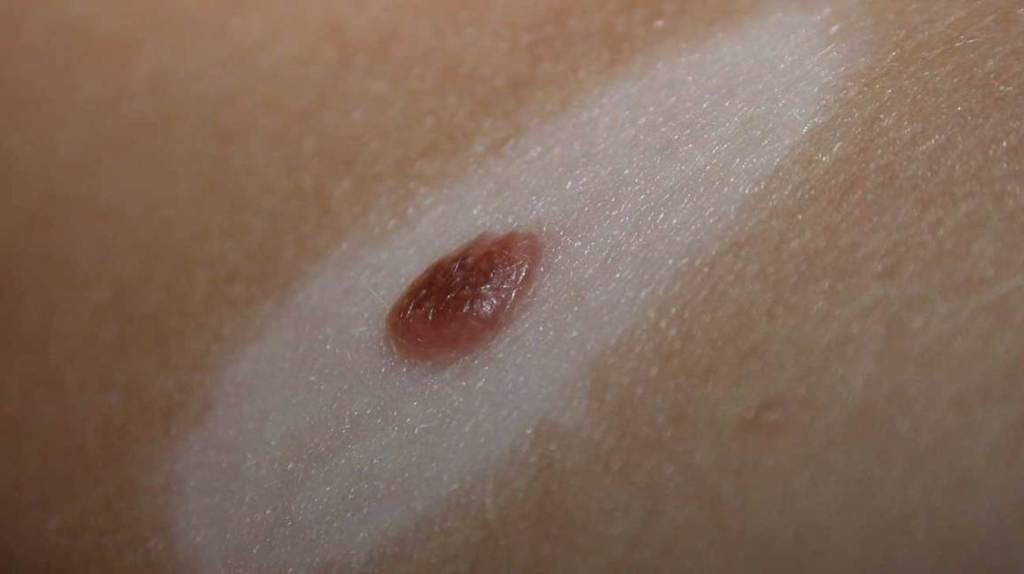
Halo Nevus: It is a mole surrounded by a white ring or halo. It is considered an immune response and affects children and young adults alike. It does not require treatment; however, it may be an early sign of vitiligo.
Breaking News: Has Researcher David Paltrow finally discovered a cure for vitiligo?
David Paltrow, an unconventional vitiligo researcher, has recently hit the news with his claim that he has discovered the real cause of vitiligo…according to him, it has nothing to do with melanin.
He is also claiming that by targeting this underlying cause, he is able to cure vitiligo in 45 days flat.
Check out his video presentation below:
