Vitiligo is a de-pigmenting skin disorder that is caused by the selective loss of melanocytes. This loss of melanocytes results in the discoloration of the skin patch. The conditions that lead to the onset of this disease include oxidative stress and environmental factors. This disease is an autoimmune disorder and is not life-threatening itself, but there are chances for vitiligo to be associated with other underlying diseases.
There has been a clinical association detected in the patients of vitiligo and thyroid disorders. The evidence is that T cells that lead to thyroid disorders are found in the periphery of affected lesions of vitiligo patients. Some cases of vitiligo have also been found in association with other endocrine disorders and various underlying diseases.
Self-Examination
One should be highly advised to see a dermatologist if any abnormality or skin discoloration is noticed. There are also a few at-home observations that can be recommended for the diagnosis of vitiligo and its relation with a thyroid disorder and underlying diseases.
The following signs can be detected through self-examination:
- Faded or dull patches on the skin
- Swelling of the lymph nodes, especially in the neck area
- Pain, itching, or lesion formation on the affected areas
- Discoloration inside the nose’s mucous membrane and mouth
Signs and Symptoms
If there is a suspicion of thyroid disorders in a vitiligo patient, then the next step is to check whether the thyroid disorder is hyperthyroidism or hypothyroidism.
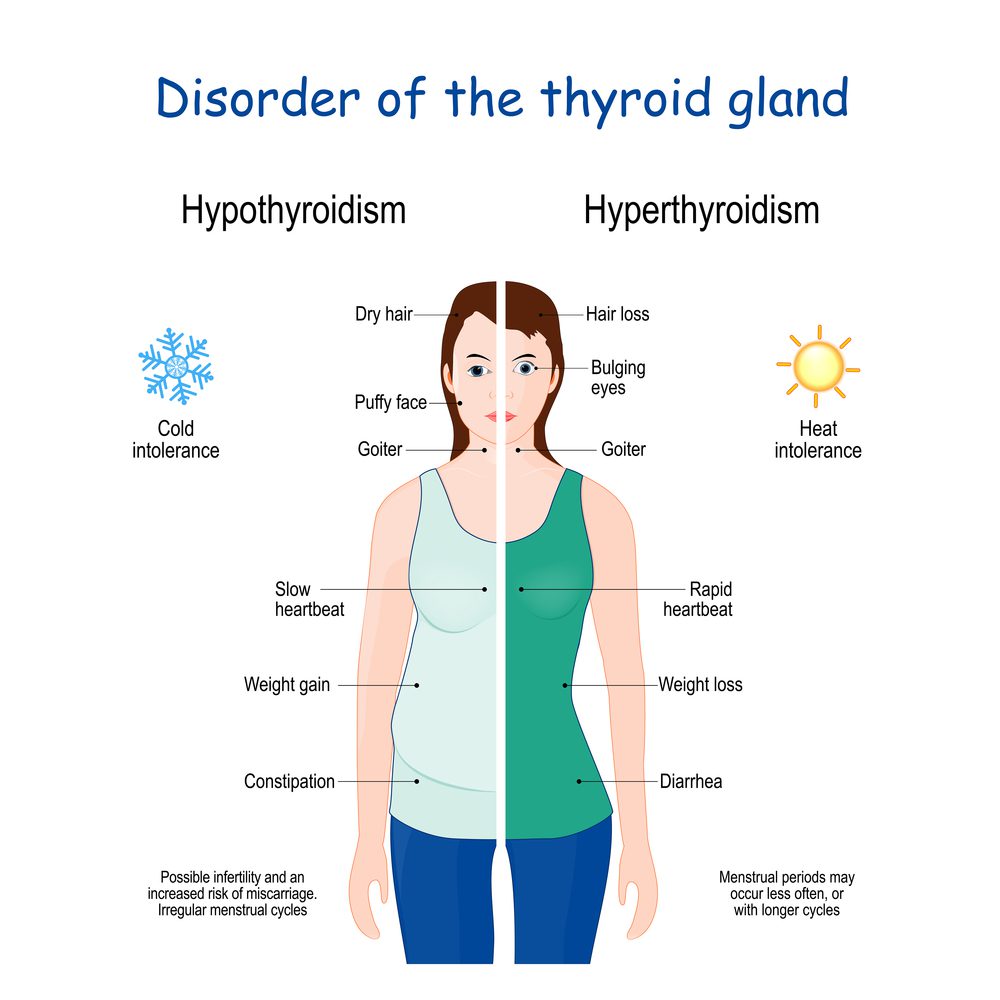
Patients with hypothyroidism and vitiligo will suffer from the following symptoms:
- Weight gain
- Hair loss
- Cold intolerance
- Dry skin
- Constipation
Patients with hyperthyroidism and vitiligo will suffer from the following symptoms:
- Nervousness
- Heat intolerance
- Skin Irritation
Tests for Vitiligo associated with other disorders
Skin biopsy is done to out rule the possibilities of any cancers associated with vitiligo. In this procedure, a small tissue of the skin is extracted and examined under the microscope for the confirmation or exclusion of other underlying diseases such as skin cancers, etc. The following blood tests will be recommended by your medical practitioner for screening of a thyroid disorder:
- Complete blood count test (CBC)
- Thyroid stimulation hormone (TSH) test
- Reverse T3 (RT3)
- Folate/B12
Conclusion
There are chances of association of vitiligo with other autoimmune disorders, especially thyroid disorders. Once you are diagnosed with this disease, you should seek medical help as soon as possible. Early treatment can control the vitiligo’s spread and severity.
References
- Narita, T., Oiso, N., Fukai, K., Kabashima, K., Kawada, A., & Suzuki, T. (2011). Generalized vitiligo and associated autoimmune diseases in Japanese patients and their families. Allergology international : official journal of the Japanese Society of Allergology, 60(4), 505–508. https://doi.org/10.2332/allergolint.11-OA-0303
- Fan, K. C., Yang, T. H., & Huang, Y. C. (2018). Vitiligo and thyroid disease: a systematic review and meta-analysis. European journal of dermatology : EJD, 28(6), 750–763. https://doi.org/10.1684/ejd.2018.3449
- Baldini, E., Odorisio, T., Sorrenti, S., Catania, A., Tartaglia, F., Carbotta, G., Pironi, D., Rendina, R., D’Armiento, E., Persechino, S., & Ulisse, S. (2017). Vitiligo and Autoimmune Thyroid Disorders. Frontiers in endocrinology, 8, 290. https://doi.org/10.3389/fendo.2017.00290
- Bae, J. M., Lee, J. H., Yun, J. S., Han, B., & Han, T. Y. (2017). Vitiligo and overt thyroid diseases: A nationwide population-based study in Korea. Journal of the American Academy of Dermatology, 76(5), 871–878. https://doi.org/10.1016/j.jaad.2016.12.034
- Akay, B. N., Bozkir, M., Anadolu, Y., & Gullu, S. (2010). Epidemiology of vitiligo, associated autoimmune diseases and audiological abnormalities: Ankara study of 80 patients in Turkey. Journal of the European Academy of Dermatology and Venereology : JEADV, 24(10), 1144–1150. https://doi.org/10.1111/j.1468-3083.2010.03605.x
- Hadi, A., Wang, J. F., Uppal, P., Penn, L. A., & Elbuluk, N. (2020). Comorbid diseases of vitiligo: A 10-year cross-sectional retrospective study of an urban US population. Journal of the American Academy of Dermatology, 82(3), 628–633. https://doi.org/10.1016/j.jaad.2019.07.036
Do you have a treatment for vitiligo?
LikeLike